If you experience joint pain despite medications, creams, and even physical therapy, you may be weighing your options. For people who can’t or don’t want to have joint replacement surgery, joint injections can be a long-term (though not permanent) solution for managing pain.
People get joint injections when they need immediate pain relief from acute or chronic joint injury. Joint injections are minimally invasive, and use a needle to deliver treatment directly into the joint.
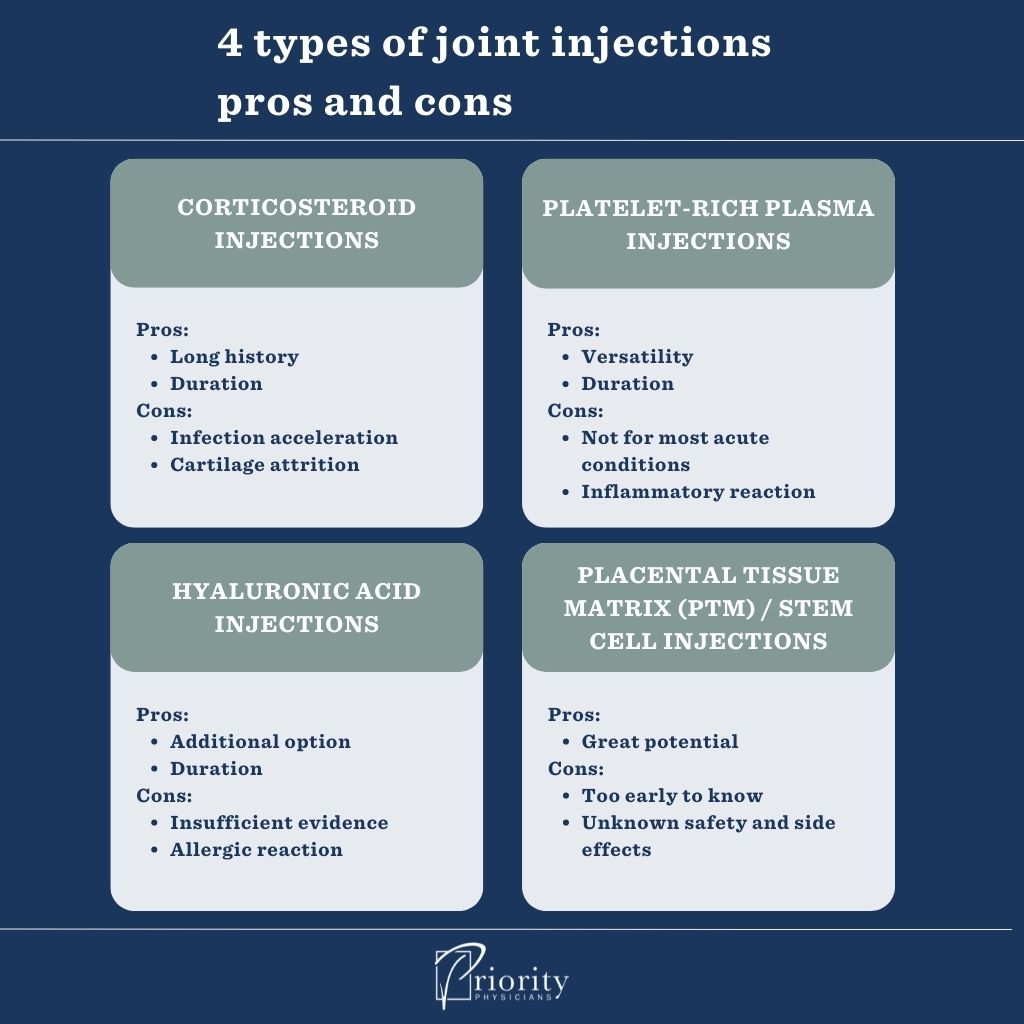
In this post, we’ll discuss four types of joint injections, plus the pros, cons, and myths of each.
What Are the Differences Between the 4 Types of Joint Injections?
There are four types of joint injections:
- Corticosteroid
- Platelet-rich plasma (PRP)
- Hyaluronic acid
- Placental tissue matrix (PTM) or stem cells
They each have their pros and cons, and there are even some myths involved. By knowing the different types of joint injections, you’ll be able to make an informed decision about which is right for you.
Corticosteroid Injections
Corticosteroids are medications that reduce inflammation in the body, making them effective options for reducing painful, damaging inflammation in joints. However, corticosteroids can weaken muscles and tendons if injected into these tissues, even leading to ruptures. For this reason, corticosteroid injections are best used in joints.
When a patient has acute pain and swelling from a joint injury or arthritis, their doctor can inject a corticosteroid directly into the joint, most commonly the knee but also the hip, shoulder, spine, hands, and feet. In addition to a steroid, the injection also often contains a local anesthetic like lidocaine to decrease pain even faster.
Pros of Corticosteroid Injections
Long history. Corticosteroid injections are the most common type of joint injection and have been around the longest. They have a long track record and much evidence and experience behind them.
Duration. Corticosteroid injections can last for several weeks, months, or even longer.
Cons of Corticosteroid Injections
Infection acceleration. If the pain and swelling in a joint are from an infection, a corticosteroid injection will accelerate that infection. Corticosteroids suppress immune activity, so it’s important to be sure an infection isn’t the cause of the joint pain.
Cartilage attrition. Frequent use of corticosteroid injections can contribute to cartilage deterioration in the joint, worsening the source of the problem. Patients should only receive one corticosteroid injection per joint each quarter, or four total per year.
Platelet-Rich Plasma Injections
Platelet-rich plasma comes from your very own blood. It starts with a regular blood draw, like you would get for any blood test. Then in a laboratory, a centrifuge spins your blood to separate the blood plasma from the blood serum.
The plasma is rich in platelets, which are one of the body’s healing mechanisms. They have anti-inflammatory properties and act as the body’s bandages. If you cut your knee, for example, platelets rush to the area to clot the blood, stop the bleeding, and form a scab.
Once isolated, this platelet-rich plasma can be injected to help injured tissues grow and repair. Platelet-rich plasma injections have been tried and tested in various musculoskeletal conditions, including chronic tendinitis, plantar fasciitis, and osteoarthritis.
Pros of Platelet-Rich Plasma Injections
Versatility. Unlike corticosteroids, platelet-rich plasma injections can treat ligaments and tendons as well as joints.
Duration. Platelet-rich plasma injections usually last for months rather than weeks, with six months being the average.
Cons of Platelet-Rich Plasma Injections
Not for most acute conditions. Typically, rehab is recommended instead of platelet-rich plasma injections for most musculoskeletal conditions, such as acute injuries. However, platelet-rich plasma injections may be used to treat chronic injuries, such as chronic tendonitis, or injuries in high-performing athletes who need to return to play quickly.
Inflammatory reaction. Platelet-rich plasma injections can irritate the surrounding tissues, causing an inflammatory response almost like an allergic reaction. If an inflammatory response occurs, it’s usually within a week of the injection.
Hyaluronic Acid Injections
It may sound counterintuitive to inject an acid into a painful joint, but hyaluronic acid is a remarkable, soothing substance that the human body produces on its own. It helps keep your tissues hydrated, your skin resilient and flexible, and your joints moving smoothly. The hyaluronic acid used in injections comes from the combs of roosters.
Hyaluronic acid first found its niche in treating patients with knee osteoarthritis, and its use has since expanded. SYNVISC is one of the most common brands of hyaluronic acids used in joint injections.
Pros of Hyaluronic Acid Injections
Additional option. If corticosteroid injections don’t work or stop working, hyaluronic injections are an alternative joint injection option patients can try for pain and swelling relief.
Duration. Hyaluronic acid injections tend to last longer than cortisone injections, 6–12 months or more.
Cons of Hyaluronic Acid Injections
Insufficient evidence. Based on existing studies, there is limited evidence that hyaluronic acid injections provide benefit. This doesn’t mean they don’t work, but that research hasn’t conclusively demonstrated that they do.
Allergic reaction. Hyaluronic acid injections can cause temporary, short-term pain and swelling in the joint, but the main con to watch for is an allergic reaction.
Placental Tissue Matrix (PTM) / Stem Cell Injections
The concept behind PTM or stem cell injections is that stem cells are pluripotent, meaning they can morph into any other type of cell. When you’re born, you have many stem cells which differentiate into muscle cells, bone cells, liver cells, etc. as you grow. The older you are, the less potential your stem cells have to become different kinds of cells.
Stem cells can come from placental tissue, other people, or yourself (if you’re younger). Some companies also synthetically derive stem cells for use in injections. The hope is that after injection, stem cells will recognize where they are — say, in the joint cartilage — and begin to differentiate into more of that type of cell, repairing and regenerating the damaged area.
Pros of PTM / Stem Cell Injections
Great potential. If stem cell injections work, they have enormous potential to help repair and protect joints, in addition to other uses.
Cons of PTM / Stem Cell Injections
Too early to know. We don’t yet know if stem cell injections work, meaning they could be a huge waste of money for people trying them.
Unknown safety and side effects. We don’t yet have enough information to know whether stem cell injections are safe and what side effects they may produce.
Myths of PTM / Stem Cell Injections
Because of the way stem cells work, it’s easy for suffering patients to believe that this treatment is a cure-all for almost any type of injury or disease. And unfortunately, some companies and people do take advantage of that belief, injecting stem cells into almost any part of the body a patient will allow.
But there isn’t much evidence demonstrating the safety or efficacy of stem cell injections, or how doctors should use them. Yet. A lot of good research is in progress, but at present it’s just too early to know.
While stem cells seem to have great potential, we need to get a better understanding of their use so we know that they’re both safe and effective.
Next Steps for People Who Want Joint Injections
If you think you might benefit from one of these types of joint injections, the first step is to speak to your doctor. They can advise you on which type of joint injection would be best for your situation.
Most primary care physicians can give cortisone injections right in their offices. However, platelet-rich plasma and hyaluronic acid injections will require you to see a sports medicine doctor or an orthopedic surgeon.

